Improving Maternal and Newborn Health in the DRC: The Importance of MPDSR in Crises
As we prepared to join a call to discuss this blog, Christine was delayed—not by a scheduling conflict, but by the sound of bombs exploding outside. This is the reality many people face in eastern DRC, where we never know what the next day will bring. Yet, amidst the violence, one truth remains: pregnancy and childbirth don’t stop in times of crisis, and neither should access to high-quality maternal and newborn health services.
A Fragile System in Crisis
Even before the escalation of violence in early 2025, the DRC’s health system was fragile. With fewer than one health worker per 1,000 people, maternity care was already under strain. Years of inadequate funding, low wages, and insufficient training left the system unable to meet even basic health needs. As a result, the DRC is among the countries with the highest maternal mortality ratios in the world.
Today, the situation has become even worse. Displacement, declining access to health facilities, and rising maternal health risks are leaving thousands of pregnant women vulnerable. The situation has been made worse by the sudden halt of U.S. aid funding, which sustains certain health programs including support for health workers, facilities, and essential medical supplies. In such circumstances, preventable deaths are an inevitable tragedy.
The Role of MPDSR
In this context, Maternal and Perinatal Death Surveillance and Response (MPDSR) becomes an essential tool for addressing the growing number of preventable deaths. In 2015, the DRC introduced MPDSR systems to track, analyze, and learn from every death to improve care and prevent future losses. However, the system is not fully functional and key questions like “What went wrong?”, “Could this death have been prevented?”, and “What can we do better next time?” often remain unanswered.
In stable settings, we’ve seen MPDSR used to help improve care and ultimately reduce mortality. However, in conflict zones in eastern DRC, where instability complicates healthcare delivery, implementing MPDSR becomes more challenging. With fragile health information systems and poor documentation, tracking deaths—especially among displaced populations—is nearly impossible. Nevertheless, MPDSR remains an opportunity to help uncover root causes of deaths and offer insights to inform life-saving interventions.
Opportunities to strengthen MPDSR systems: A Study in North and South Kivu
To better understand how MPDSR is working in the DRC, our team, as part of the EQUAL research consortium, undertook a study across six districts (health zones) in North and South Kivu provinces (read the research briefs in English or French). We visited urban, stable rural, and unstable rural districts, interviewing 109 people, from hospital staff to community leaders, and assessed existing systems that document how maternal and perinatal deaths are identified, reported, and reviewed.
Existing Systems: What’s Working and What Isn’t
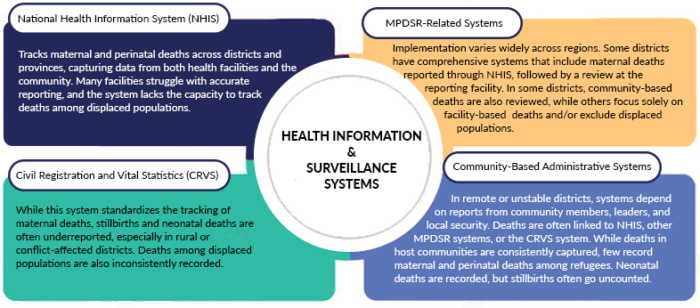
We discovered that while some districts have strong health information and surveillance systems, others are failing to capture the necessary data. Several systems are used for tracking maternal and perinatal deaths:
- National Health Information System (NHIS): Tracks maternal and perinatal deaths across districts and provinces, capturing data from both health facilities and the community. Many facilities struggle with accurate reporting, and the system lacks the capacity to track deaths among displaced populations.
- MPDSR-Related Systems: Implementation varies widely across regions. Some districts have comprehensive systems that include maternal deaths reported through NHIS, followed by a review at the reporting facility. In some districts, community-based deaths are also reviewed, while others focus solely on facility-based deaths and/or exclude displaced populations.
- Civil Registration and Vital Statistics (CRVS): While this system standardizes the tracking of maternal deaths, stillbirths and neonatal deaths are often underreported, especially in rural or conflict-affected districts. Deaths among displaced populations are also inconsistently recorded.
- Community-Based Administrative Systems: In remote or unstable districts, systems depend on reports from community members, leaders, and local security. Deaths are often linked to NHIS, other MPDSR systems, or the CRVS system. While deaths in host communities are consistently captured, few record maternal and perinatal deaths among refugees. Neonatal deaths are recorded, but stillbirths often go uncounted.
Barriers to Effective MPDSR in Crisis Contexts
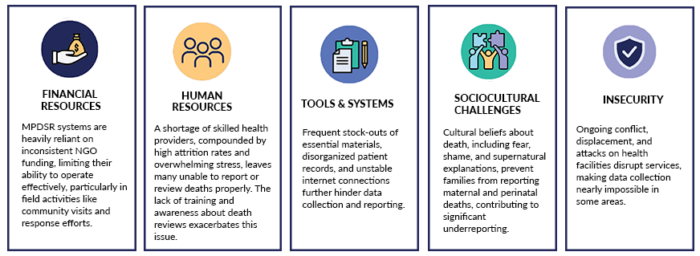
There are many barriers to MPDSR implementation in conflict-affected districts of the DRC. Financial constraints, a shortage of skilled health workers, and the strain of insecurity are just the start. Sociocultural challenges also play a role in underreporting deaths, especially in rural districts where death is sometimes seen through cultural or supernatural lenses.
As one key informant in the Katwa district noted, “Some people don’t understand the purpose of the death review. Some see it as an accusation and so they try to defend themselves. This creates a defensive atmosphere, which sometimes undermines the process.”
A health worker in Mweso added “We’re working under stress, we’re not going to work as we should, because all the time we’re thinking about how to escape the war.”
Promising Practices and the Way Forward
Despite the challenges, we identified several promising practices that have been helpful in improving maternal and perinatal death surveillance in North and South Kivu provinces. These practical insights can be applied in other crisis settings as well:
- Engage Local Actors: Empowering Community Health Workers (CHWs) and local leaders is critical. In some districts, CHWs facilitate household visits and collaborate with local authorities to incorporate maternal and perinatal death reporting and reviews into the community, making the process more efficient and effective.
- Frame MPDSR as Quality Improvement: In regions where MPDSR has been positioned as a quality improvement tool—rather than a system for assigning blame—health workers have been more willing to participate. This approach fosters transparency and accountability, which strengthens the entire health system.
- Leverage Technology: In some conflict zones, innovations like mobile technology, satellite communication systems (VSAT), and solar-powered tools have been critical in maintaining real-time reporting and efficient data collection, even in districts with poor infrastructure.
- Strengthen Coordination: Collaboration with local leaders, including those in displaced communities or districts under the control of armed groups, has helped keep systems functioning even in the face of insecurity.
Based on everything we learned, EQUAL is now working to support efforts to strengthen community-based MPDSR approaches that leverage these existing systems, and the promising practices identified.
A Call to Action
As the crisis continues in the DRC, it feels more important than ever to call on governments, NGOs, donors, and the global health community to invest in adapting and implementing MPDSR systems in crisis settings. As our research highlights, improving maternal and perinatal death surveillance in conflict-affected regions like eastern DRC requires flexible and context-specific systems. There is no one-size-fits-all solution, but what’s clear is that strengthening systems like MPDSR is critical and should not be overlooked.
As one of our colleagues put it, “If this is what we call resilience, then something’s wrong with resilience.” We cannot accept this harsh reality as the status quo. It’s time for change that saves lives, even under the most challenging circumstances. Let’s create systems that don’t just track deaths but actively work to prevent them.
This blog was written with support from Alicia Adler.
On Monday, 24 March, EQUAL and the Global MPDSR Technical Working Group hosted a webinar on MPDSR in Humanitarian Contexts. The webinar presented the latest research, real-world adaptations, and strategies for implementing MPDSR in the most challenging environments. With insights from Eastern DRC, Gaza, and Sudan, speakers discussed how MPDSR remains a vital tool for improving care and saving lives, even in acute emergencies. Watch the webinar below.